Most of us are familiar with the stories of diseases that devastated the world in the medieval or early modern days. Disease of Justanian, the Black Death, and the list goes on. However, many modern pandemics are forgotten, or at least diminished to minor outbreaks in our minds. That is one of the reasons we found ourselves surprisingly unprepared facing COVID-19: Pandemic seemed to be something from a distant past, or from a distant place. But pandemics in the last 200 years affected us in a way that was not experienced before, due to the ever increasing global interactions. Here are some cases of the modern pandemics, and what we can learn from them.
Cholera: How a disease and our responses to it changed in the modern era
Cholera is a bacterial disease that causes severe diarrhea and dehydration, and it is transmitted through contaminated water and food. The first cholera pandemic occurred in India in 1817, which soon became a worldwide outbreak, and since then there have been six more cholera pandemic, the last being the outbreak during from 1961 to 1975. Because of poor public sanitation and terribly managed water supplies, the first four pandemics were particularly deadly in large cities of Europe, including London and Paris, claiming more than 10,000 lives in one outbreak. The disease was also spread through growing international interactions, such as British troops in India, waves of immigration, and global maritime trade, showing how the characteristics of the modern era, including urbanization and globalization, can contribute to the spread of diseases. During the third pandemic, however, an English physician John Snow discovered that contaminated water was the agent of spreading disease, and efforts to improve public hygiene and water systems were made in later pandemics — making cities in the West mostly unaffected by the last two cholera pandemics. People have learned how to deal with cholera, and cholera is no longer a disease that would cause an unstoppable pandemic.However, this does not mean cholera is a disease only in the past. To these days, many countries in poverty, which cannot guarantee access to clean water, are suffering from this disease. The most recent cholera outbreak was in Yemen in 2017, where a civil war interrupted water supply. The outbreak is still ongoing, and has become the worst epidemic in the history, with more than 2 million cases suspected. Cholera still threatens numerous people’s lives to this day.
Third Plague Pandemic: The return of the Black Death… and the emergence of modern epidemiologyThe disease was named this way because it was the third major bubonic plague pandemic in history — the first being the Plague of Justinian and the second the Black Death. The plague first appeared in China in 1855, and spread to the world in 1894, when Hong Kong was affected by the disease. The Third Plague spread even more quickly than the Black Death due to cargos containing rats and fleas, but the development of modern medicine prevented the same result as the Black Death. A bacteriologist Alexander Yersin quickly identified the bacteria. The fact that rats and fleas were responsible for the spread was also found, and many modern treatment methods, including use of quarantine, antibiotics, and insecticides, were followed. As a result, the Third Plague was not as fatal as the Plague of Justinian or the Black Death. Nevertheless, the Third Plague still had a large impact on Asian countries, mainly China and India, which had fewer resources available. 12 million people in China and India died from the Third Plague, and the pandemic remained active until the 1960s.
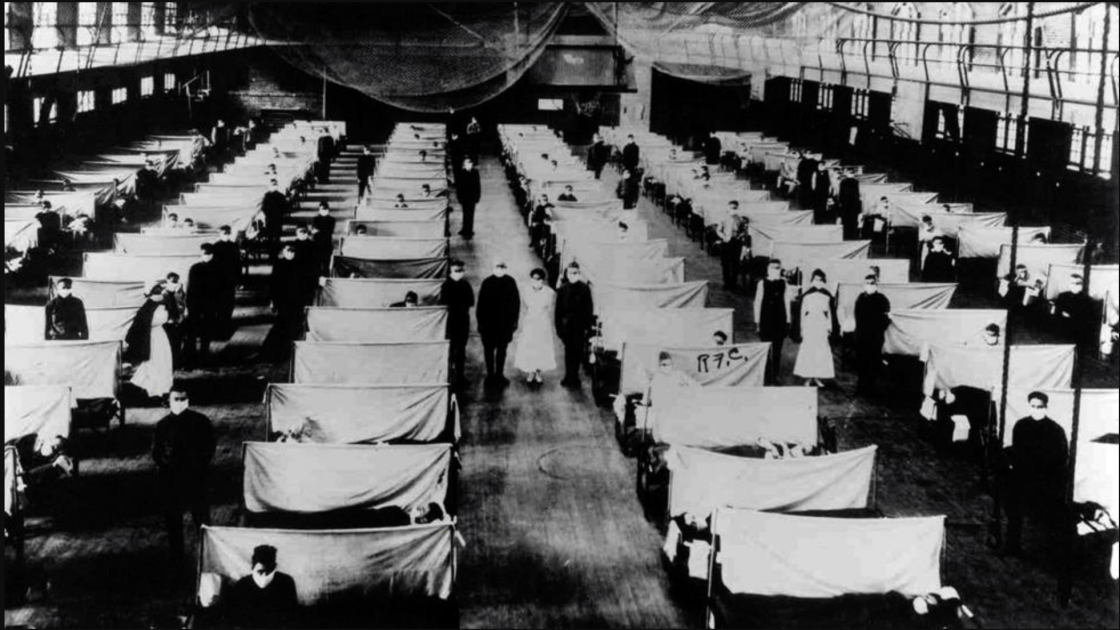
Spanish Flu: The most deadliest disease in modern history We are all kind of familiar with influenza outbreaks, due to recurring flu seasons and flu shots, but the Spanish flu was different from other influenza pandemics that occurred in the 20th century for many reasons. First, the Spanish flu showed a high mortality rate for young people from 20 to 45, while most influenza mostly kills people who are very young or very old. Soldiers fighting in the WWI, who were already weakened by malnutrition, overcrowdedness, and mental stress, were particularly vulnerable to the disease. The Spanish flu also showed unusually high mortality rate and infection rate: The estimated number of the infected was 500 million, and the estimated death toll was at least 50 million (according to CDC). The vaccine was not found during the outbreak, and many of the characteristics of the Spanish flu are still in mystery. Only recently it was identified that the influenza virus was H1N1 type.Another unique phenomenon during the pandemic was that the governments around the world were mostly trying to cover up the outbreak because they feared that the flu might discourage people from fighting in WWI. In Britain, France, Germany, and the United States, the seriousness of the disease was minimized and the media was censored. Only in Spain, which did not participate in WWI, the flu received attention, which made the disease called “Spanish flu” although the pandemic was no less serious in other countries. Partly as a result of these attempts, the Spanish flu was largely forgotten during the 20th century, but now it is getting a huge attention because of the recent COVID-19 pandemic.
Encephalitis Lethargica: The unsolved medical mystery
Encephalitis lethargica is an infectious disease affecting the brain that results in speechless, motionless condition, serious lethargy, and symptoms similar to Parkinson’s disease. The pandemic of encephalitis lethargica occurred around the world from 1915 to 1926, coinciding with the Spanish flu, and more than a million people died as a result. The cause of the disease is still unknown as well as the exact method of transmission and effective treatments. Fortunately, there has been no outbreak after the end of the pandemic. However, without knowing the cause and treatment of encephalitis lethargica, we are still unprepared for another outbreak, if it would return. The mystery of encephalitis lethargica still remains unsolved.
Smallpox: From the disease that killed the most people to the first eradicated disease
If the pandemics above give you fear and worry, the case of smallpox may give you hope. Throughout history, smallpox killed countless numbers of people, killing 300 – 500 million people only in the 20th century. However, the history of smallpox is also marked by the human efforts to prevent smallpox. Inoculation, in which a material taken from the infected was inserted or rubbed on scratches on skin, was the first prevention method for smallpox. Inoculation resulted in smallpox infection, with the possibility of death, but it was much milder than actual infection. Later, Edward Jenner invented the first smallpox vaccine using cowpox in 1796. By the 20th century, smallpox was almost eliminated in most industrialized countries because of vaccination, although smallpox continued to devastate developing countries, especially India and countries in Africa. The first effort to eradicate smallpox globally was made in 1950, and the Smallpox Eradication Unit was established in 1966. Despite many hardships and bad conditions, intensive surveillance, containment, and vaccination were put in practice. Finally, the eradication of smallpox was declared in 1979, making smallpox the first disease to be eradicated by human effort.
Conclusion
New trends of the modern era brought about new patterns of disease outbreak, and they resulted in various outcomes. In some cases, modern medical methods effectively contained diseases that might have been more deadly otherwise; in other cases, modern medicine did little to prevent the outbreak, and sometimes the cause was not even identified. In some cases, active government actions prevented spread of diseases effectively; in other cases, governments actually made the pandemic worse, trying to cover up the diseases. In most cases, poor countries and regions were most vulnerable and suffered the most, although global actions and cooperation among countries were able to eradicate smallpox in poor countries. We don’t know to which direction the COVID-19 pandemic would head, and how it will be recorded in history. What we can be certain of, however, is that there are valuable lessons that can be learned from the history of previous pandemics. History repeats itself, but it is up to us to decide which history we will repeat.